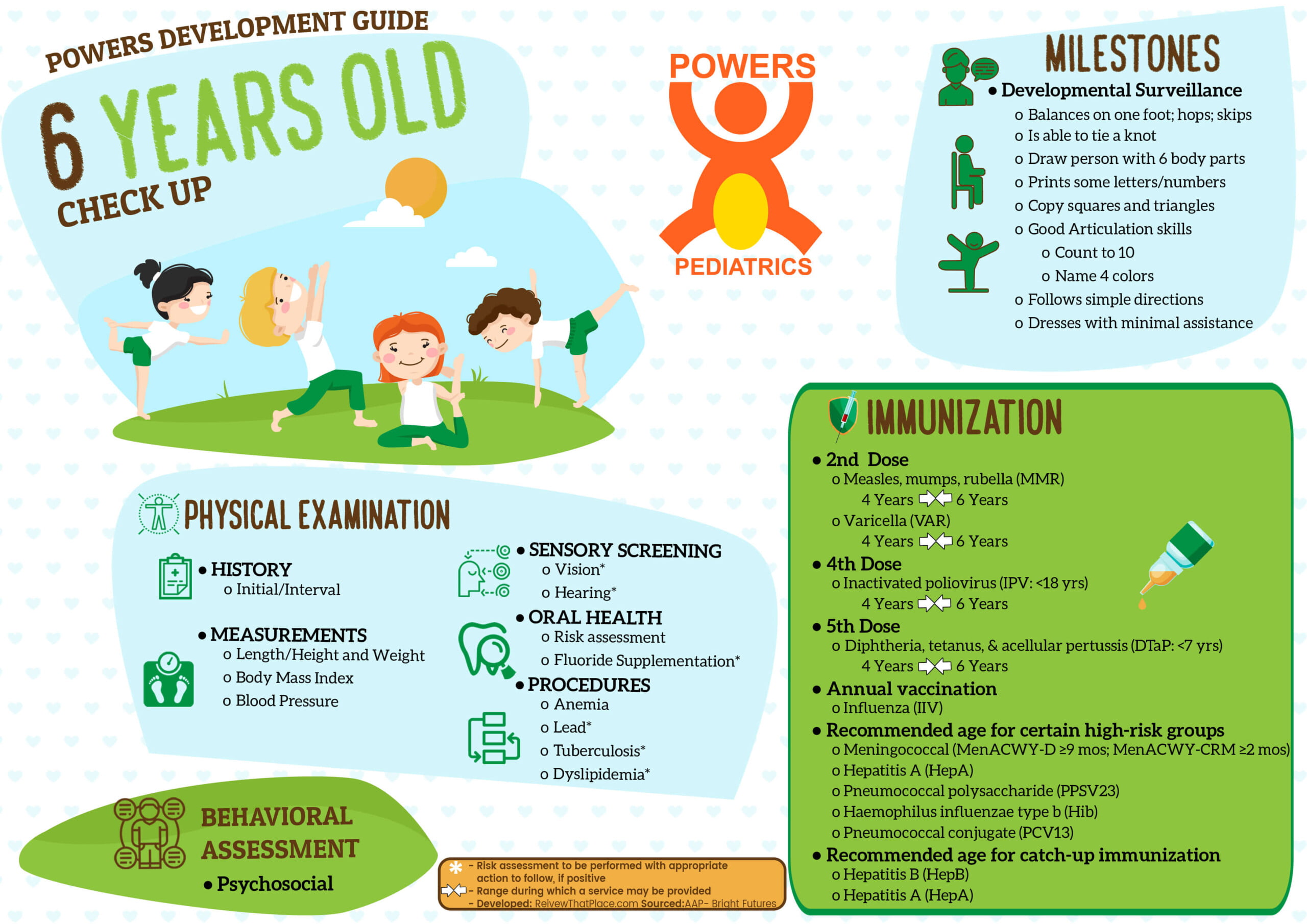
What to except during a 6 Year Old Physical?
1 DEVELOPMENTAL SCREENING
- Balances on one foot; hops; skips
- Is able to tie a knot
- Draw person with 6 body parts
- Prints some letters/numbers
- Copy squares and triangles
- Good Articulation skills
- Count to 10
- Name 4 colors
- Follows simple directions
- Dresses with minimal assistance
BEHAVIORAL HEALTH
- 2 Psychosocial/Behavioral Assessment
3 PHYSICAL EXAMINATION
14 Immunization
- 2nd Dose
- Measles, mumps, rubella (MMR)
- 4 Years 6 Years
- Varicella (VAR)
- 4 Years 6 Years
- 4th Dose
- Inactivated poliovirus (IPV: <18 yrs)
- 4 Years 6 Years
- 5th Dose
- Diphtheria, tetanus, & acellular pertussis (DTaP: <7 yrs)
- 4 Years 6 Years
- Annual vaccination
- Influenza (IIV)
- Recommended age for certain high-risk groups
- Meningococcal (MenACWY-D ≥9 mos; MenACWY-CRM ≥2 mos)
- Hepatitis A (HepA)
- Pneumococcal polysaccharide (PPSV23)
- Recommended age for catch-up immunization
- Haemophilus influenzae type b (Hib)
- Pneumococcal conjugate (PCV13)
- Recommended age for catch up immunization
- Hepatitis B (HepB)
- Hepatitis A (HepA)
6 Year Old Anticipatory Guidance
Social determinants of health
◊ Risks (neighbor hood and family violence, food security, family substance use)
◊ Strengths and Protective Factors (emotional security and self-esteem, connectedness with family)
- Teach your child nonviolent conflict-re solution techniques.
- Talk with parents/trusted adult if you are bullied.
- Within the past 12 months, were you ever worried whether your food would run out before you got money to buy more? Within the past 12 months, did the food you bought not last and you did not have money to get more?
- Contact community resources, like SNAP, for help with food assistance.
- Don’t use tobacco /e-cigarettes. Call 800-QUIT NOW (800-784-8669) for help to quit smoking. Talk with me if you are worried about family member drug/alcohol use.
- Encourage independence, self-responsibility; show affection; praise appropriately.
- Spend time with your child. Make time to talk. How are you getting along as a family? What do you do together?
Development and mental health
◊ Family Rules and Routines
◊ Concern for Others
◊ Respect for Others
◊ Patience and Control Over Anger
- Continue family routines; assign household chores.
- Use discipline for teaching, not punishment.
- Model anger management /self-discipline.
- Solve conflict/anger by talking, going outside and playing, walking away.
- What makes you sad/angry? How do you handle it?
School
◊ Readiness ◊ Established Routines ◊ School Attendance
◊ Friends ◊ After-School Care and Activities ◊ Parent-Teacher Communication
- Ensure child is ready to learn (regular bedtime routine, healthy breakfast).
- What concerns do you have about your child’s ability to do well in school?
- Tour school; attend back-to-school events.
- Be sure after-school care is safe, positive.
- Talk with child about school experiences.
- If child has special health care needs, be active in IEP process.
Physical growth and development
◊ Oral health (regular visits with dentist, daily brushing and flossing, adequate fluoride, limits on sugar-sweetened beverages and snacks)
◊ Nutrition (healthy weight; increased vegetable, fruit, whole-grain consumption; adequate calcium and vitamin D intake; healthy foods at school)
◊ Physical Activity (60 minutes of physical activity a day)
- Help child with brushing teeth if needed.
- Visit dentist twice a year.
- Brush teeth twice a day; floss once.
- Help child choose healthy eating (provide healthy foods, eat together as a family, be a role model).
- Eat breakfast; eat vegetables fruits.
- Eat when you’re hungry; stop when you’re satisfied.
- Drink milk 2 to 3 times a day.
- Limit sugary drinks/foods.
- Consider making family media use plan (www. healthychildren.org/MediaUsePlan), which can help balance child’s needs for physical activity, sleep, school activities, and unplugged time; decide on rules for media time in time left over after all other activities; take into account quantity, quality, location of media use.
- Be physically active often during the day.
Safety
◊ Car Safety ◊ Outdoor Safety ◊ Water Safety ◊ Sun Protection ◊ Harm from Adults ◊ Home Fire Safety ◊ Firearm Safety
- Use properly positioned belt-positioning booster seat in backseat.
- Teach safe street habits (crossing/riding school bus).
- Ensure child uses safety equipment (helmet, pads).
- Teach child to swim; supervise around water.
- Use sunscreen; wear hat; avoid prolonged exposure when sun is strongest, between 11:00 am and 3:00 pm.
- What would you do if a grown-up made you scared? Who could you tell? Who would help you?
- Teach rules for how to be safe with adults: (1) no adult should tell a child to keep secrets from parents; (2) no adult should express interest in private parts; (3) no adult should ask a child for help with his/her private parts; explain “privates ‘.’ Have you talked with your child about ways to avoid sexual abuse?
- Install smoke detectors and carbon monoxide detector /alarms; make fire escape plan.
- Remove firearms from home; if firearm necessary, store unloaded and locked, with ammunition locked separately.
Goals For 6 Year Check up:
- Be gentle and patient
- Get more sleep
- Make a budget
- Leave your work at the office
- Focus on self-care
- Meditate as a family
- Find an outlet
- “cell-free” zone
- Spend more time with your partner
- Take more baths
- Have a girls’/boys’ night
- Be more flexible
- See your child for who they are
- Teach your child to speak up
- Help those less fortunate
- Drink more water
- Find 30 minutes a day of “me” time
- Challenge yourself
- Focus on experiences, not things
- Make health a priority
- Start—or finish—a degree
- Inform yourself ◌ Maintain balance
- Laugh often
- Cook dinner more frequently
- Ask for help
- Have designated “cheat” days
- Stop having FOMO
- Say “I love you” more often
- A visual acuity screen is recommended at ages 4 and 5 years, as well as in cooperative 3-year-olds. Instrument-based screening may be used to assess risk at ages 12 and 24 months, in addition to the well visits at 3 through 5 years of age. (Reference) ↩︎
- This assessment should be family centered and may include an assessment of child social-emotional health, caregiver depression, and social determinants of health. (Reference) ↩︎
- At each visit, age-appropriate physical examination is essential, with infant totally unclothed and older children undressed and suitably draped. The extent of the physical examination is determined by both the reason for the visit and diagnostic considerations raised during the taking of the history. (Reference) ↩︎
- Screen, per reference. ↩︎
- Blood pressure measurement in infants and children with specific risk conditions should be performed at visits before age 3 years. (Reference) ↩︎
- A visual acuity screen is recommended at ages 4 and 5 years, as well as in cooperative 3-year-olds. Instrument-based screening may be used to assess risk at ages 12 and 24 months, in addition to the well visits at 3 through 5 years of age. (Reference) ↩︎
- Recommend brushing with fluoride toothpaste in the proper dosage for age. (Reference) ↩︎
- Once teeth are present, fluoride varnish may be applied to all children every 3–6 months in the primary care or dental office. (Reference) ↩︎
- If primary water source is deficient in fluoride, consider oral fluoride supplementation. (Reference) ↩︎
- These may be modified, depending on entry point into schedule and individual need. ↩︎
- Perform risk assessment or screening, as appropriate, per recommendations in the current edition of the AAP Pediatric Nutrition: Policy of the American Academy of Pediatrics (Iron chapter). ↩︎
- For children at risk of lead exposure, see per reference. ↩︎
- Testing should be performed on recognition of high-risk factors. Tuberculosis testing per recommendations of the AAP Committee on Infectious Diseases. ↩︎
- Every visit should be an opportunity to update and complete a child’s immunizations. (Reference) ↩︎